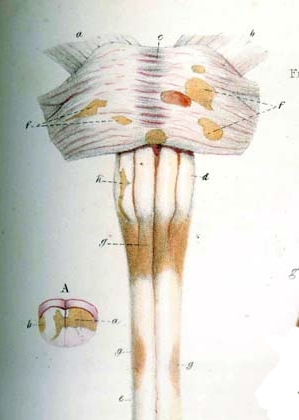
Image via Wikipedia
It's now been about 16 months since the first Multiple Sclerosis patients outside of Italy underwent the venoplasty treatment known as The Liberation Procedure to address the then little heard of vascular condition termed "Chronic Cerebrospinal Venous Insufficiency", or CCSVI for short. Discovered earlier in the decade by the Italian vascular physician Dr. Paolo Zamboni, whose published papers reported success rates previously unheard of in the treatment of MS, knowledge of the condition and its potential relationship to MS was at that time scant, with few people in the MS community having ever heard of CCSVI. Those that were aware of the vascular hypothesis were confined, for the most part, to a small group of patients actively debating the relative merits and deficiencies of the hypothesis on one somewhat obscure MS Internet forum.
Well, what a difference 16 months make. The small trickle of patients undergoing treatment has now become, if not quite a flood, then at the very least an ever-increasing cascade, and word of CCSVI has spread like a kerosene fueled inferno throughout the MS population. Indeed, the very landscape of the Multiple Sclerosis world has shifted, as seismic waves of hope, promise, and controversy have swept over the horizon. In some cases, battle lines have been drawn, and in others, alliances formed. Fairly or not, in the eyes of many MS patients, mainstream neurology and the MS societies have become the enemy, mired in an outdated medical dogma and held in the sway of Big Pharma, and interventional radiologists following in Zamboni's footsteps have been hailed as conquering heroes.
Some of the first US doctors to start performing the Liberation Procedure were soon stopped by wary hospital administrators, but a handful of interventional radiologists in the United States are still openly doing the work, and a network of physicians operating "under the radar" has formed, their names being furtively passed from patient to patient via e-mail and social networking internet sites. Internationally, clinics offering the procedure are popping up from Costa Rica to Bulgaria, and the business of CCSVI medical tourism is booming. YouTube is bursting with videos of patients displaying their post-liberation gains, and web forums are abuzz with CCSVI chatter. Nonprofit CCSVI advocacy groups have formed, and patients, after years of being dictated to, are finally enjoying the self empowerment of having their say.
Put in its simplest terms, the CCSVI hypothesis states that blockages in the jugular and azygous veins, which drain the brain and spinal cord respectively, cause a long-term disruption in the flow of blood through the central nervous system, thus causing, over a period of many years, the damage to nervous system tissues that has come to be called Multiple Sclerosis. This relatively straightforward but radical notion flies in the face of accepted Multiple Sclerosis doctrine, which states that MS is an autoimmune disease caused by an immune system gone awry, and for reasons still unknown goes on a cannibalistic attack of a patient's own tissues. Though at first glance appearing to be at odds, in some ways the two theories actually complement each other, as CCSVI offers an explanation as to how and why immune system cells, which normally are stopped from infiltrating the central nervous system, can find their way through the blood brain barrier to wreak havoc on the nervous system beyond.
So, the CCSVI revolution rockets onward, an irreconcilable force destined to redefine, at a very basic level, medical science’s understanding of one of its greatest mysteries, the mechanism behind MS and maybe even some other autoimmune diseases, right?
Well, not so fast. Despite the boundless optimism expressed by many MS patients, there are still many very legitimate questions that need to be answered about the CCSVI hypothesis and the Liberation Procedure, questions impacting both near and long-term implications for the Multiple Sclerosis universe.
On a pathophysiological level, while CCSVI does seem to answer many of the perplexing questions surrounding MS, in some very important areas the hypothesis fails to reconcile with some firmly established facts about the disease. Among the most glaring examples of these are:
- The geographic distribution of the disease, which shows that the prevalence of MS increases indisputably the further away one gets from the equator. Additionally, migrant studies show that when people move from an area where MS is common to an area where it is rarer they show a decrease in the rate of the disease, whereas migrants moving in the opposite direction tend to retain their resistance to the disease. There is also evidence that susceptibility to the disease might also be linked to the age at which migration occurs. (Click here)
- The female to male ratios of people with MS, which appears to be growing farther apart. In 1940, the ratio of women to men with MS in the US was about 2 to 1. By 2000, that ratio had grown to nearly 4 to 1. (Click here)
- The genetic factors that have been identified as being related to susceptibility to MS, though few, are all associated with genes that play a role in regulating the immune system. (Click here)
- The association of MS with Epstein-Barr virus. Although over 90% of the population is infected with EBV, recent research has shown that people who don't have EBV do not get MS. (Click here)
- According to CCSVI theory, which states that blood refluxing back into the CNS causes the inflammation that is a hallmark of MS, it would seem that the amount of inflammation would continue to increase with the age of the patient. Instead, the inflammation seen in MS typically reaches its apex in the early relapsing remitting stage of the disease, but falls off dramatically when the disease enters the later, progressive stage. Patients who start out with progressive disease (PPMS), though generally older at the time of diagnosis, typically show very little evidence of CNS inflammation. (Click here)
Although it is difficult to understand the above factors in terms of CCSVI, they do not invalidate the theory. MS is an extremely heterogeneous disease, suggesting that multiple factors are likely at work, and that these factors very likely change from individual to individual. In fact, what we call MS may not be one disease, but rather a collection of diseases that share some common elements. A research effort called The Lesion Project (click here, page down to "Heterogeneity of the disease") has identified four distinct lesion types through the postmortem examination of MS nervous system tissues. The project has further found that each patient only exhibits one type of lesion, and that some of the lesion types surround blood vessels while others do not.. This evidence suggests that different disease processes may be at work, and it could very well be that CCSVI plays a major role in some forms of what we call MS, but a lesser role, or no role at all, in others.
This also helps explain the variance in the effectiveness of the liberation treatment from patient to patient. Some patients see dramatic improvements in their condition, sometimes almost immediately after having their veins unblocked. Other patients exhibit no benefit from the procedure, and some even get worse. Dr. Gary Siskin, an interventional radiologist doing the Liberation Procedure in Albany, New York, has publicly stated that one third of his patients see dramatic improvements, one third minor improvements, and a final third no improvements at all.
Dr. Siskin also stresses the importance of doctors managing patient expectations, as the vast majority of materials on the internet (YouTube videos, patient testimonials, etc.) paint an overly positive picture of the results of liberation. This isn't due to any kind of deception on the part of MS forum members or YouTube posters, but is simply a function of human nature. Patients who exhibit dramatic improvements are far more likely to publicize the outcome of their procedures than those who experience disappointing results. It's very important that patients go into venoplasty with reasonable expectations.
The tools and methodology for both the detection and treatment of CCSVI have so far demonstrated sometimes serious deficiencies. On the detection side of things, the most common noninvasive imaging techniques, MRV and Doppler sonogram, have both proven to be less than reliable in identifying the venous defects associated with CCSVI, returning both false-positives and false negatives. Doctors and patients alike have noted that their preprocedure imaging very often does not match up with what is actually found during the catheter venogram procedure, which is the gold standard for imaging venous abnormalities.
The handful of imaging studies done have produced widely varying results, some detecting nearly universal evidence of CCSVI in MS patients, and others finding scant evidence of CCSVI at all. While some of these discrepancies can be attributed to variances in methodology and operator competence, I believe the overall reason for these vastly different findings falls on the failings of technology. So far, the only reasonably reliable noninvasive imaging method appears to be Doppler sonography done according to very specific protocols designed by Dr. Zamboni, but even the results of testing done to these exacting standards at times proves to be unreliable, and, according to the doctor who performed my recent sonogram using the Zamboni protocols, are still somewhat subjective. The physical abnormalities being attributed to CCSVI are hardly subtle, and one would think, given the advanced state of medical technologies, that a variety of instruments and methodologies would be able to pick them up. Apparently, this is not the case, and it is imperative that better imaging techniques be developed, as it is simply not feasible to perform invasive catheter venograms on every patient suspected of having CCSVI.
At a recent CCSVI symposium attended by many of the interventional radiologists most experienced with the Liberation Procedure (click here for report), it was apparent that the Liberation Procedure itself is still in its early infancy and is a very much a work in progress. Many of the presenting radiologists commented on the steep learning curve involved with doing the procedure, and the opinions of these very accomplished physicians varied widely on subjects as fundamental as the proper size of balloons to be used during venoplasty, whether or not stents should be used to prop open blocked veins, and even what constitutes a treatable stenosis. Dr. Sclafani, who performed my attempted liberation (blockages were found but were unable to be addressed, click here for more info) has in no uncertain terms called this an age of discovery. If CCSVI is indeed shown to be a causative factor in Multiple Sclerosis, it's very likely that veins other than the jugular and azygos (such as the lumbar and vertebral veins) play a role in the disease, and presently there is no way to address blockages in these vessels. It's very important that patients be cognizant of these factors when making the decision whether or not to undergo liberation.
Many patients who opt for venoplasty alone (without the use of stents) experience restenosis of their treated veins, necessitating a repeat procedure. If the initial procedure was done locally, and was covered by insurance, this might not pose much of a problem. On the other hand, if the patient traveled thousands of miles, and spent the $10,000-$20,000 often required for travel and treatment, such a repeat performance may prove to be impossible, turning their initial procedure into a financial disaster.
Patients who have stents implanted in their blocked jugular or azygos veins are entering the realm of the unknown, as all of the stents currently in use were designed to be implanted in arteries, which anatomically are extremely different from veins. The only other patient population that regularly has stents implanted in their veins are end-stage hemodialysis patients, who suffer from extremely serious kidney disease. Studies done on the failure rates of these stents are not encouraging, often finding a 50% failure rate after one year (click here for an extensive study, or here for a chart summarizing its results ). I'm certain that the stresses placed on stents during the dialysis process are much different than those placed on stents implanted in CCSVI patients, so the validity of the comparison may questionable. Still, all of the currently available stents were designed primarily for use within the chest cavity, where they are not subject to the constant bending, twisting, and torque that they experience when implanted in the extremely flexible human neck. For patients determined to improve their hemodynamic blood flow and stand a better chance at avoiding restenosis, or whose veins simply don't respond to repeated attempts at ballooning, stents do offer a viable alternative to balloon venoplasty. Clearly, if CCSVI does prove to be an important piece of the MS puzzle (and I believe it will), stents specifically designed for use in the jugulars will be sorely needed.
In conclusion, it has certainly been an interesting 16 months. While much has been learned in regards to CCSVI, there is much more that has yet to be learned. Although some questions have been answered, many more have been raised. A robust treatment trial of the Liberation Procedure that includes sham procedures would be the quickest and most effective way to answer most of these questions. Researchers at the University at Buffalo are currently conducting such a trial, albeit a small one, limited to 30 subjects . Unfortunately, as of today, no other such trials have yet been funded.
CCSVI offers MS patients tangible hope, a commodity in perilously short supply before news of the hypothesis made its way through the Multiple Sclerosis community. Quite literally sick of, and from, taking the drugs that many MSers know are doing nothing to address the underlying cause of their disease, CCSVI has been embraced by patients with a fervor rarely seen in modern medicine. In some cases, I fear that the strength of these convictions has at times overwhelmed reason. I fully understand the desperation felt by those afflicted with this damned disease, as I am subject to it myself. Still, it should be at the forefront of every patient's mind that while the past year has been very encouraging, CCSVI and its role in MS has by no means been proven.
I personally made the choice to attempt liberation because of the severity and aggressiveness of my disease. Each patient must assess their own risk/reward ratio, keeping in mind that many of the questions surrounding CCSVI will likely be answered sooner rather than later, and the techniques used to address blocked veins will mature at a rapid pace, as physicians gain experience and work their way up the learning curve. Quite likely, Liberation Procedures done 12 months from now will be significantly different from those done today, and patients who can afford to wait before embarking on liberation will surely benefit from the accrual of knowledge and the perfection of technique that can only come with time.

marc, thank you.
ReplyDeleteyour posts are always full of insight. it feels great to read a fellow ms-er toning down the hype of ccsvi and at the same time keeping our hopes high in its potential. we need to keep it real. i don't know of any recent medical progress out of the well established peer reviewed research and i have no doubt that the scientific community will overcome any obstacles due to special interests. what we need is some patience ... even if we have no time to wait.
"If I have ever made any valuable discoveries, it has been owing more to patient attention, than to any other talent." Isaac Newton (1642 - 1727)
Marc,
ReplyDeleteIf only....
"If I have ever made any valuable discoveries, it has been owing more to patient attention, than to any other talent." - Isaac Newton
I'm worried about the dishonesty in the CCSVI camp - I understand the blood flow issue because I can feel it & have vague illnesses to show for it. MS is elsewhere in the family so that may be the link.
I see CCSVI as a starting point because we can see and monitor that now. More help will come, and people like you will make that happen.
Im worried about medical ethics because they're visibly stretched at the best of time, so why should this change overnight because CCSVI gets mentioned?
Cost is a huge worry, so are blood flow problems upstairs (all modern societies, across every group in the land, except for todays "modern western society."
Price = Value
We've had the onslaught of sales, some even mention CCSVI.
Yes, I agree, CCSVI is just one focus. I still doubt healthcare will give up their golden goose, and money has a way of influencing and justifying under the radar of donkey clinical science.
Difference levels of good intentions but very little good will & certainly none outside business circles.
Clinical science is Big Pharmas messiah, remember, they invented it's excellence.
A scot draws the first MS lesions and Scotland wins highest prevalence award. Im still trying to work out how my mouse got MS after a visit to the vet.
Skill will surely improve, so will resistent to treatment and business contributions to clinical science.
Great post as ever, helps me restore a little balance.
Mark, great post.
ReplyDeleteI encourage you to watch Dr. Hubbard's presentation at the Haacke event regarding MS and CCSVI theories, or read the transcript, which I posted on my Facebook notes. Hubbard's CCSVI theory is slightly different from Zamboni's, and he posits that perhaps our nerves, deprived of proper blood flow, have gone into what he calls a "compromised" state, like a hibernation, and function normally again when proper blood flow is restored. Haacke mentioned a study of rats that reduced blood flow to their nerves and the nerves ceased to function. Once blood flow was returned, the nerves began functioning again, so there is evidence that blood flow is related to nerve function. Hubbard believes that if the nerve axon has been deprived of blood flow for too long, it is likely to be permanently dead, and the procedure will not restore it. This may explain why some people have dramatic results, while others have only minor improvements.
There was also a British study which found that a drop in temperature contributed to an increase in heart attacks. If temperature is related to vascular issues, could this perhaps explain why there is a greater prevalence of MS in cooler climates?
Here are some links to investigate:
Dr. Hubbard's presentation on the theories of MS and CCSVI: http://www.facebook.com/note.php?note_id=146646562024535 (That's the transcript...video link is included.)
The British study:
http://www.lifelinescreening.com/health-updates/healthy-you/heart-health/cold-weather-boosts-heart-attack-risk.aspx?SourceCd=LETT-681
Another excellent read is Dr. Ashton Embry's Open Letter to Alberta's Minister of Health, which calls for a retraction of AHS's August 6 statement regarding MS and CCSVI because it was riddled with inaccuracies and fear-mongering. Dr. Embry's letter presents research data and facts regarding CCSVI.
ReplyDeletehttp://www.facebook.com/note.php?note_id=456172859918
Hello Marc,
ReplyDeleteI'd love to have a live discussion with you on the other facts about MS (ie. epstein barr, females and geography. Oh and genetics). I had a very interesting conversation with a dear friend of mine about emotional stress/pain which has been shown and continues to show an impact on MS symptoms but also the vascular system.
I know when I experience stress and emotional pain, my symptoms really take hold and are vicious. If I am relaxed and at ease, my symptoms are minimal. A lot of fellow MSers have had such emotion embedded deeply into their past. I know my own has been extreme.
I live south of you in Maryland, near one of those handful of interventional radiologists who is a friend of Dr. Dake. I am to be treated very soon for the CCSVI I have been found to have. He's also jointly working with their MS department on a real, valid study that will examine stent use versus non-stent use.
In their hope, a number of MS patients are calling this a cure. I do know of friends that have had very good results and some that are "so so" (this may also have to do with the stage of the disease and how long a person has been symptomatic).
I really do love reading your blog very much and your writing style. I'm writer myself. :)
I also video blog on youtube and am the administrator and founder of the Maryland USA MS CCSVI Group on Facebook, where I publish links to your writings and blog. The Dr. down here that is performing liberations also is an admin and at least monitors the site. :)
http://www.facebook.com/pages/Maryland-USA-MS-CCSVI-Group/114648478563437?ref=sgm#!/pages/Maryland-USA-MS-CCSVI-Group/114648478563437?ref=sgm
I keep track of as many news broadcasts as I can find on www.youtube.com/msccsvinews
My own meanderings and writing are in the Notes section. I wrote recently to Dr. Katherine Knox who is doing one of the MS Society funded studies. She wrote back and was actually cordial. She connected me with her research assistant for discussion.
Marc, I really DO enjoy what you do. I hope someday I get to meet you.
http://www.youtube.com/watch?v=fy7ipDAyXtI
ReplyDeleteHi Marc,
ReplyDeleteSince you added this to your page at 2:33am,I'll guess that you hadn't yet seen the SIR position statement issued today:
http://www.sirweb.org/news/newsPDF/Release_JVIR_MS_final.pdf
I took the liberty of emailing this to a local research university and the local chapter of the MS Society. Perhaps I'm overly enthusiastic, but this is the most encouraging medical groups position statement that I've seen yet. I've gone so far as to suggest that the MS Society stop their passive studies (by Neurologists!), and redirect the $$$$'s to Interventional Radiology groups. Maybe I'm delusional but I want to climb (as if)to the nearest mountaintop (in Florida...not) and scream.
Dear MS Society Director,
I wanted to share this with you. I sent this note to all of the Vascular/Radiologists/Neuro docs at ?????.
This is a bold statement by the Society of Interventional Radiologists issued today.
While it's understandable that Neurologists have 'owned' our disease up until now, the fact is that CCSVI is
essentially vascular in nature. What is very frustrating for those of us suffering with this disease, the MS Society's funding for research was directed to Neurologists, Neuroradiologists, Neurovascular doctors.
Thankfully, the SIR is calling for studies on CCSVI and interventional MS therapies.
It's not too late for the MS Society to rethink the passive studies that they've funded. If some of the current studies are halted and funding redirected to IR groups, we'd be one step closer to a world where real treatment happens!
Fortunately, the SIR feel the same degree of urgency that we, the patient community, also feel.
I know you're the messanger but I'd appreciate you sending this message to your leadership.
Thanks , Chris Weller
~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~
Dear Dr. XXXXXXX,
I'm very enthusiastic to see this today:
'Interventional Endovascular Management of Chronic Cerebrospinal Venous
Insufficiency in Patients with Multiple Sclerosis: A Position Statement by the Society of Interventional Radiology'
The profound conclusion of this Position paper is an urgent call to action:
SIR believes that the completion of high-quality studies on CCSVI and interventional MS therapies should be considered an urgent research priority by investigators, funding agencies, and MS community advocates. SIR, through its Neurovascular and Venous Service Lines, is moving rapidly to catalyze the development of the needed studies by bringing together expert researchers in imageguided venous interventions, neurology, central nervous system imaging, MS outcomes assessment, and clinical trial methodology.
http://www.sirweb.org/news/newsPDF/Release_JVIR_MS_final.pdf
I'm a resident of ??????????? and willing to volunteer my services if ?????
would pursue a study into CCSVI in Multiple Sclerosis. These are exciting times for the MS community.
Hi Mark,
ReplyDeleteSince you added this to your page at 2:33am,I'll guess that you hadn't yet seen the SIR position statement issued today:
http://www.sirweb.org/news/newsPDF/Release_JVIR_MS_final.pdf
I took the liberty of emailing this to a local research university and the local chapter of the MS Society. Perhaps I'm overly enthusiastic, but this is the most encouraging medical groups position statement that I've seen yet. I've gone so far as to suggest that the MS Society stop their passive studies (by Neurologists!), and redirect the $$$$'s to Interventional Radiology groups. Maybe I'm delusional but I want to climb (as if)to the nearest mountaintop (in Florida...not) and scream.
Dear MS Society Director,
I wanted to share this with you. I sent this note to all of the Vascular/Radiologists/Neuro docs at ?????.
This is a bold statement by the Society of Interventional Radiologists issued today.
While it's understandable that Neurologists have 'owned' our disease up until now, the fact is that CCSVI is
essentially vascular in nature. What is very frustrating for those of us suffering with this disease, the MS Society's funding for research was directed to Neurologists, Neuroradiologists, Neurovascular doctors.
Thankfully, the SIR is calling for studies on CCSVI and interventional MS therapies.
It's not too late for the MS Society to rethink the passive studies that they've funded. If some of the current studies are halted and funding redirected to IR groups, we'd be one step closer to a world where real treatment happens!
Fortunately, the SIR feel the same degree of urgency that we, the patient community, also feel.
I know you're the messanger but I'd appreciate you sending this message to your leadership.
Thanks , Chris Weller
~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~
Dear Dr. XXXXXXX,
I'm very enthusiastic to see this today:
'Interventional Endovascular Management of Chronic Cerebrospinal Venous
Insufficiency in Patients with Multiple Sclerosis: A Position Statement by the Society of Interventional Radiology'
The profound conclusion of this Position paper is an urgent call to action:
SIR believes that the completion of high-quality studies on CCSVI and interventional MS therapies should be considered an urgent research priority by investigators, funding agencies, and MS community advocates. SIR, through its Neurovascular and Venous Service Lines, is moving rapidly to catalyze the development of the needed studies by bringing together expert researchers in imageguided venous interventions, neurology, central nervous system imaging, MS outcomes assessment, and clinical trial methodology.
http://www.sirweb.org/news/newsPDF/Release_JVIR_MS_final.pdf
I'm a resident of ??????????? and willing to volunteer my services if ?????
would pursue a study into CCSVI in Multiple Sclerosis. These are exciting times for the MS community.
Marc, whenever I finish reading one of your posts, I feel a profound sense of relief at having heard from someone who combines intelligence, judgement, and thoroughness in addressing the topic at hand. This post was no exception. You perform a great service for our community. I am very grateful for what you do so well.
ReplyDeleteJudy
Thank you again Marc for your excellent discussion.
ReplyDeleteI'm grateful to the SIR for their position supporting robust research into CCSVI and MS. They are stepping up where others have let us down.
Recent sunshine on the obscene salaries of the MS society has made their modest investment and their CCSVI study selection process seem slimy.
The editors of the journal best mispronounced rushed to publish and promote the "wrath of kahn" and the inept and "Dope" studies - 6 weeks, no peer review- really???---rather than seriously apply their own talents to examining this intriguing discovery, which appears to hold such promise, as directed by the Stanford dean.
It's time to stop the wizard of Oz imitation and promote the application of resources to do an expedited, large scale, proper examination of this complex, multifactorial problem. the curtain has been pulled back by the scruffy little dog. Thanks, Toto!
I have been liberated. I have a stent. I am getting better for the first time since diagnosis. Need better technology to resolve all my issues, don't want to wait for the naysayers to get a grip. The anatomical facts dictate the pathology. It's true.
Hi Marc,
ReplyDeleteThank's again for your very informative blog, which I read with great interest each and every time. You expose the facts, the implications, without pre-conceived ideas nor bias, even if MS is pretty agressive in your case.
It is clear to me that MS is multifactorial and for my case, genetics played a huge role - my mother had MS, her father before her, one of her aunt, one of her cousin, and the daughter of one of my cousin - 6 persons in 3 generations. Which of MS or CCSVI has genetic origins? The answer is yet to come... However, none of my siblings have MS, but my sister and my oldest brother have Oculo-Pharyngea Distrophy, which my mother also had. Unfortunatly, she had the whole works...
This being said, CCSVI also makes great sense to me, since immuno-modulation therapy worked for me - Betaseron - only for a couple of years, and I always feel, since day one, this pressure in the back of my neck and a pulsating pain from the base of the nape, irradiating to the forehead via the middle of the skull - which corresponds to the Jugular Gulf and the Superior Sagittal Sinus trajectory - especially before my MS symptoms exhacerbations.
And to Judy, I also have stress related symptoms increases; stress do cause blood vessels' vasoconstriction, worsening the stenosis and blood reflux that may be present.
And on the opposite, Lisinopril, which is a high blood pressure medication, currently under study for it's potential beneficial effect on MS symptoms, is a vasodilatator, promoting a better blood flow. However, some of it's components may have anti-inflammatory properties.
Thank you again Marc for your wonderful posts and so generously answering my technical questions in order to improve my own little bilingual blog, simply called IVCC/CCSVI-ALAIN, which is only at it's infancy.
Hi Alain,
ReplyDeleteI've actually taken Lisinopril and in my case it did a small miracle. Three days on it and I had regained all my balance and could feel the bumps on the linoleum floor under my feet. I could wiggle my toes when I'd stopped being able to move them.
I do have high blood pressure it justified me taking it.
Sadly a good percentage of people have a very bad uncontrollable cough as a side affect. For the physical good it did, I began to and could not stop coughing till I pulled all my abdominal muscles.
Sadly, I had to stop taking it. I believe this allows the tissue around the veins to relax a bit and allow more blood to flow though.
I now take a similar medicine but it does not have the same dramatic effect.
Serge-thanks for your comments, and I really like the Newton quote…
ReplyDeleteMiyagi-money and medicine quite often are a dangerous mix, and can form an unholy alliance. Unfortunately, this is the system we are stuck with, but keep in mind that the profits threatened (neurologists, pharmaceutical companies) by CCSVI are matched by the prophets promised (interventional radiologists, medical device companies). Thus the tug-of-war we now see playing out. Would be an interesting show if our asses weren't on the line…
Dawn-thanks for your comment, and for the extremely interesting links. You've done good work in putting up the Hubbard transcript, which contains much good material. I do wish that the neurologists and intervention radiologists would stop the carping and start acting like adults. I know several neurologists who are open to the idea of CCSVI, and especially welcome that attention is finally being given to theories other than autoimmunity. So they are not all evil…
As for the "hibernation" theory, I'd be careful about that one. Rats are part of a species (rodents) in which hibernation is known to occur, whereas it is unknown in Homo sapiens. Although I've known a few who I swear have been in hibernation for most of their lives…
I do agree with Hubbard's "swamp" theory. Clearly, if the junk is not getting flushed from the brain, bad things could result.
The British study is interesting, but I don't think it really relates to CCSVI or MS. The defects being found in CCSVI are congenital, making it hard to see a link between cold weather and CCSVI. Furthermore, most MS patients are extremely heat sensitive, and one would think that if cold played a part in the disease, then heat would actually help rather than hinder MS patients.
Judy-thanks for your comments. Since the vascular defects being seen in CCSVI are congenital, stress and emotional trauma could not be there genesis, but could certainly exacerbate an already existing vascular problem. We know that stress can cause cardiac problems, so why not neurologic ones?
ReplyDeleteNice work on your Facebook pages, looks like you're covering all the bases. As I've written before, the amount of education and empowerment that CCSVI has spurred among MS patients is a victory in and of itself.
Anonymous-love the Robo suit video. Look for it in an upcoming "bits and pieces" post. Thanks.
Chris-your attempt at outreach is admirable, but once awarded, I don't think the funds provided to researchers by the MS societies can be withdrawn. Luckily, it looks like the provincial governments in Canada may step in to fill the void, and start funding treatment trials sooner rather than later. Not soon enough for many of us, but at least we know that they are coming.
Let me preface this following statement by saying that I am by nature a cynical man. The statement put out by the SIR is very encouraging, but one must also remember that the group represents doctors who stand to make a quite a fortune if CCSVI proves to be the real deal. Neurologists and the MS societies are frequently bashed because of the perception that they are acting (or not acting) in large part due to their own financial interests. Let's not forget that this phenomenon is not the province of neurologists alone…
Judy-thank you very much for your extremely kind words. I do my best, but look forward to the day when I can turn my attentions to happier subjects…
ReplyDeleteCarol-first of all, a big congratulations on your successful liberation, and tremendous wishes for continued improvement.
As for the salaries of the officers of the MS Society, I must say that people doing the same job in the private sector earn a considerable amount more than what is being paid to the MS Society higher-ups. I'm certainly shedding no tears for the president of the MS Society and her $500,000 salary, but keep in mind that mid-level managers of Wall Street firms would turn their nose up at such a paltry sum. A private sector CEO running an organization of the size and scope of the NMSS could easily earn three or four times as much in base salary alone, before bonuses and stock options kick in.
Not to defend obscene salaries for anyone, but the fact is that those working at nonprofit, from bottom to top, often do so for far less money than employees of for-profit businesses.
I'm also compelled to defend what many consider the undependable, the dreaded "khan paper". While the tone of the paper may at times be demeaning, its substance deserves some attention. The authors do bring up some very salient points regarding some apparent disconnects in CCSVI theory with est. knowledge regarding MS. Could the paper have been more polite and politic? Certainly. Is Dr. Khan a jackass? Probably. Still, these deficiencies do not invalidate the intellectual points he makes.
Having said all that, I do fervently wish that robust treatment trials would be started immediately. All of the questions the confusions could then be dealt with quite expeditiously.
Alain-thanks for your well-informed post. Your family history certainly does point to a genetic connection related to MS, and would seemingly be a great case study for geneticists working on the problem. It's a bit hard to see CCSVI as a genetic problem, since so many different types of abnormalities are being found. Not to rule out a genetic-CCSVI connection, because we are really just at the very infancy of the learning process. Your point regarding stress and vasoconstriction is a good one, and the effects of stress could certainly exacerbate an already existing vascular dysfunction. Glad my advice was of help to you, please feel free to ask if any more is needed.
Judy-the inventor of Tysabri (who later came out against the drug) has been wanting to test lisinopril on MS patients for some time, but can't get the requisite funding because the drug is off patent. Another example of our completely broken medical research model at work…
Just a quick note about my responses, above: in rereading them, I noticed a few typos. Please forgive me, as I use voice recognition software to "type", and it sometimes just doesn't get things right. I am guilty of not sufficiently proofreading, but it's late, I'm tired, and it's time for the kamikaze to go sleepy sleep…
ReplyDeleteWhat do I love about your blog? I am regularly copying and pasting references made by you and others into Google so I can expand my knowledge base about this unrelenting intruder. This is more enlightening than any of the graduate level classes I've ever taken! Thanks!!
ReplyDeleteMB
Marc,
ReplyDeleteThank you for your kind wishes. I wish your problem were as straightforward. We both will benefit when the device makers and imaging guys develop the technology to better address the problems associated with the azygous vein.
I must say I do feel personally injured by the lisinopril guy you speak of and the editors i mentioned as well as Dr Kahn. who are all on record very publuically trying to shut down research into CCSVI. "move along folks, nothing to see here, veins can't possibly be involved in MS, take my pill". Their pills don't work for me. I need that research very much. I am working hard to promote proper studies, educate practitioners, establish a useful registry and get out ALL the good the bad and the ugly about CCSVI and MS. Why are they at war with the IRs? Their behavior needs to be examined fully. They successfully shut it down in the 1980's. How many more have to suffer needlessly?
Without accelerated clinical treatment trials, more and more people will be treated by people who are not fully qualified or not cooperating with patient outcome studies, or worse. The variable outcomes that result will just further clog the system and increase risk, as pts need 2-3 procedures from different sites to get it right. We need the leading IRs in the top institutions to do the proper controlled studies and then publish and teach the best techniques, as they work with industry to improve the technology.
The hold-outs for the failed immune theories i referenced above have a moral and academic duty to cooperate with the IRs in their respective institutions and get to the bottom of this!
In fact I believe they should have to defend their behavior in front of their academic senates. They are reaching into a department where they are not experts and telling that department that they cannot offer their services to patients who carry the diagnosis of MS. It is indefensible.
Hey WCK
ReplyDeleteGreat post, to once again get people thinking.
Love your profound honesty.George C. Ebers geneticist at Oxford is hot on the trail of the Vit D study which shows lack of D inutero=venous and immune/bone malformations and immune system challenges hence the "auto-immune snowball that some us have on board.If the precursor hormone D "switch" is Off on our DNA which when we have MS all multi-factorial,multi-causal campers coming in to "play". We are living on the "cusp" of the unfolding theatre of discovery.I am now "following" on you blogspot and invite you to my blog http://ruth-a-n.blogspot.com/
hugs from BC Canada:)
Another well thought out informative post - and I agree with another commenter who suggested you watch the Hubbard presentation (it's on my blog too) which answers at least one of your questions.
ReplyDeleteI'm wondering if other have seen this yet - from the American Academy of Neurology no less! Acknowledgment of the role of vascular disorders in MS. About time!
http://www.neurology.org/cgi/content/abstract/74/13/1041
Mark, Dr. Hubbard said the nerves were in a "compromised" state ("hibernation" was indeed in reference to the rats). While humans do not hibernate per se, our bodies will respond to certain situations, such as starvation or meditation, with decreased metabolic activity, decreased oxygen consumption, muscle relaxation, and decreased hormone production. If the nerves are starved for blood flow, could it be that they are going into a reduced state of function?
ReplyDeleteYes, CCSVI is congenital! That means CCSVI precedes onset of MS and could indeed be a causal factor.
Does colder weather contribute to an exacerbation? (Wasn't it Nancy Davis who had her first MS attack while skiing? LOL! Well, she also had a very stressful situation, a bad marriage and a broken leg.) I am sensitive to cold. My feet and legs spasm in colder weather. Alas, I am also sensitive to heat. I got hit with a double-whammy. I need to move to a city where it is always 72 degrees!
MB-thanks for your comment, glad that you find this blog educational. It is for me, too…
ReplyDeleteCarol-thanks again for your thoughts, we certainly both could benefit from some advances in technology. It turns out now that my problem is very likely a muscle bundle impinging my right internal jugular, which may require traditional open neck surgery to address. Even my abnormalities are abnormal. Just lucky, I guess…
I can understand your frustrations with the "anti-CCSVI" neurologists and publication editors. I've reread the khan paper, and again, aside from the demeaning tone of the wording, many of the issues he raises are legitimate and do need to be explained. Having said that, just because there are issues that aren't understood doesn't mean that CCSVI research should not move forward, and quickly.
Although the words of some neurologists are reprehensible, I also find the lack of curiosity on the part of many of the interventional radiologists that are chomping on the bit to start doing liberation procedures also to be a bit disturbing. At the symposium I attended, there was very little discussion of how and why opening veins might be helping patients, and most of the IRs in attendance seemed more concerned with how they could get a piece of the liberation pie than with the actual neurologic implications of the procedure.
There's lots of money in them there veins, and as you said, many unqualified physicians just can't wait to start doing the catheter procedures regardless of their lack of experience in working on CNS veins. As much money as the Neuros and the Pharma companies stand to lose because of CCSVI, the IRs and medical device companies stand to gain. Unfortunately, on all fronts, it's mostly about the money…
The current state of unregulated chaos could very well lead to some very unfortunate outcomes which could adversely impact the entire CCSVI movement. At the very least, the amount of patients getting treated without any method of tracking or following up on them isn't helping to prove the validity of the CCSVI hypothesis. As you mentioned, many patients are requiring multiple procedures to address their problems, much to the dismay of the patients themselves, and their bank accounts.
Ruth-thanks for your comments, and the theory that vitamin D deficiency during gestation might contribute to the multifactorial causes of MS is very interesting. I'll have to do some digging on that one myself. And I will definitely visit your blog…
ReplyDeleteMs Andisue-I did watch the Hubbard presentation, and Dr. Hubbard does make some very valid points. I think we all share his frustrations with neurologists who are so entrenched in one way of thinking that they feel threatened by a theory that is outside of their comfort zone. As the saying goes, if you're a hammer, you see only nails. Well, now the hammers are being presented with screws.
The abstract you link to is indeed a cause for optimism, especially since one of the authors is Timothy Vollmer, one of the top MS Neuros in the country. Thanks for the contribution…
Dawn-it's certainly within the realm of possibility that nerve cells, in the absence of proper blood flow, could go into a reversible state of compromised functionality. I suppose the question would be, just how long can they stay in that compromise state without suffering actual structural damage. My guess would be not too long, but who knows? Recent advances in reviving patients who in the past would have been declared dead illustrate just how much we don't know about cell degradation.
I've no doubt that colder weather can contribute to MS exacerbations, as any kind of stress is known to do so. However, this wouldn't explain the preponderance of MS in colder climates when compared to warmer climates, or the evidence illustrated by migration studies.
I think the perfect city for you would be San Diego, which has some of the best weather in the world. It's also quite beautiful there, although during the one weekend I in San Diego I was kept awake by barking sea lions in the Cove outside my hotel window…
Love your blog, WcK;
ReplyDeleteTo play a bit of devil's advocate: you quoted Dr. Siskin to put a damper on things. However, when questioned by the audience at the conference, he practically confessed to under-treating (albeit in the spirit of being responsible in these early stages of a novel treatment). Dr. Petrov and Dr. Sinan both had about a 90 success rate - and Dr. Sinan did it under a prohibition on stents but with very aggressive ballooning of the valves.
I keep the faith that they will figure out a solution for you!
Nick-if memory serves, Dr. Siskin said that after watching some of the presentations, he thought he might be undertreating, but in the actual slides he presented he appeared to be much more aggressive in treating upper jugular stenosis than either Petrov or Sinan.
ReplyDeleteAs for success rate, the other docs didn't really quantify what success is. I can't comment on the Kuwaiti results, since I have had no contact with any of the patients treated there, but my own contacts with patients who have been treated in Bulgaria lead me to believe that a 90% success rate is something of an overstatement, unless some temporary slight improvements are included in the mix. Albeit I'm working from a small sample size.
This conversation just underscores the importance of some kind of attempt to track the long-term condition of patients, which seems to be sorely lacking from almost all of these efforts.
The differences in approaches between the three doctors was rather striking, and the Kuwaiti success rate without stents, and also without directly addressing upper jugular stenosis, is intriguing if indeed it is accurate. And the size of those balloons…!
Thanks for keeping the faith on a solution for me, hopefully there is a solution for all of us lurking somewhere out there in in the mists, but getting ever closer to our grasp…
You're right, Mark, I don't think cold weather easily explains the greater prevalence of MS above the 40th parallel. The best argument may be Vitamin D deficiency, and I look forward to more studies on that issue.
ReplyDeleteHow long do the nerves survive in their reduced state of function is a good question. I've seen people with the disease for two decades experience dramatic results, and yet others who have had it just as long experience only minor improvements. I read an article about a 70-something year-old woman who had MS for 50 years, and she doesn't need a cane anymore to walk. (But for having it so long, her progression seemed mild. Heck, some 70-somethings without MS need canes.) So I don't think that time is the sole factor, especially since we know the venous malformations are congenital. Why do some people exhibit MS symptoms as teenagers, while others don't have symptoms until 40? Does the severity or location of the stenoses play a role? Or the strength of the endothelium? Is there some other agent at work--a greater or lesser prevalence of certain molecules in the blood? Diet and exercise? Environmental factors? So many questions, no easy answers. Future research will hopefully help determine what reasonable results each patient can expect.
On a completely different note--researchers recently discovered that the gene HLA-DR plays a role in MS as well as Parkinson's. I began looking at genetic links between the diseases because my father has Parkinson's and I have MS. Although HLA-DR has an auto-immune function, so I am not certain how this contributes to the CCSVI argument. Do you have any thoughts on this?
Ooh, here's something interesting. "Gene Variant May Increase Severity of MS"
ReplyDeletehttp://www.aan.com/press/index.cfm?fuseaction=release.view&release=853
And here's an abstract of Dr. Simka's soon-to-be published study. He found venous blockages in 97.1% of 381 MS patients.
ReplyDeletehttp://www.facebook.com/?ref=home#!/notes/ccsvi-transverse-myelitis/dr-simkas-article-correlation-of-localization-and-severity-of-extracranial-venou/155041464507435
And apologies for spelling your name incorrectly! I grew up with a Marc, I should know better...
***dont understand how congenital malformations can transform.
ReplyDelete***dont understand how canada would refute claims of CCSVI and be so against it when prescribing Sadavax there is no problem
***dont understand how my symptoms can change by the minute. Either there's damage or there's not. Why numb hands at 12:01 and not at 12:15?
***dont understand why heat literally cripples me and then when i cool off get my strength back.
***dont understand why stress can do to me what heat does to me.
***dont understand why liberation did nothing for me yet can make one gal go from a 6.0 edss to 3.5.
***dont understand why people on TIMS post how excited they are about getting the treatment and then afterwards you dont hear anything.
***dont understand why if there was something that could help us that some neuro's wouldnt want to know or learn about it.
***dont understand why wine makews my mom's face flush.
***dont understand why mustard or balsamic vinegar makes my forhead sweat.
***dont understand why out of 300 spartans I am the one with the MS.
***dont understand why my friend is so physically strong and then woke up today and cant button his shirt because he so weak but MS was ruled out.
***dont understand why my other friend healthy as an ox fell to the ground crippled after getting on an airplane completeley strong and healthy and by her own accord until the flight was over and she tried to get out of the seat.
***dont understand the randomness of life.
***dont understand why my wife would get hospitalized witha nasty 9mm kidney stone the night before the kids go back to school.
***dont understand how the Kamikaze know so damn much about evertything.
***I guess i just dont understand...
GREEK
Okay, a question. If CCSVI is so related to MS, what would be the effect of exercise on MS? Would it increase the back flow and thus illness (as blood is pumped all around faster) or would it make the veins open out more?
ReplyDeleteMany of us have relapsing/remitting MS. It is so hard to know what makes things better or worse unless you take the long view. I've been able to exercise for the past few months and am much better. What is the cause/effect? Am I able to exercise because my disease is sleeping, or is my disease sleeping because I am able to exercise?
This is the problem with the short term results from CCSVI...
One reason that CCSVI changes with age is that some lesions contain mesenchymal cells which are a susceptible to hormones and proliferate at times of your life where hormones are active. puberty, pregnancy, menopause. this correlates w/ MS spikes. so your stenosis waxes and wanes.
ReplyDeleteExtreme exercise may indeed be a problem. many MSers report "Tomato head". This is a circulatory, hemodynamic problem, like congestive heart failure, which also causes transitory peripheral neuropathy.
I just found your blog WCK. Neither pro nor con, THAT'S refreshing..............thank you!!
ReplyDeletejust recently recieved your blog and wanted to comment on the ccsvi....my wife in a wheel chair now for 2 years continues her decline and is losing the battle to m.s.....every medicene has been useless and she refuses to try any "new" ones....the last one tysabri made her sick yet on docs orders she took it for over 16 months....my wife and i met dr. hubbard in brooklyn in early aug at a symposium and we will be flying out to san diego in early oct to have the liberation done.mentally this is the last stop for her. she is at the point now where she has no hand control ,constant pain, and is starting to suffer mentally very quickly now.bathing and other "simple" daily routines she could due herself are all gone now. i am her constant care taker and because of this we are suffering terribly financially. i pray that the liberation is successful enough to give her continued hope and a reason for living. your article on your blog gave her great encouragement and she is more confident than ever. thank you for the good news. hope to give you better news in about 5 weeks.
ReplyDeleteThanks again, as always, for an informative and well-written post. My mom and I were watching on line and were thrilled to hear your question asked, despite it not getting any kind of definitive answer from the panel.
ReplyDeleteYou are of course right on the mark saying that CCSVI treatment clincs will be opening up on every street corner, with the quality of treatment questionable at best. This makes me furious as I believe that this is happening precisely as a result of mainstream medicine tyring to put the brakes on patients getting tested and treated. All the reputable doctors are now going to be involved in trials, while the not-so-reputable will be treating desparate patients.
Zamboni had a terrific point that some MS patients should be treated out of compassionate grounds, but I don't think anyone else was listening. Everything I have heard says that balloon agioplasty is an extremely safe procedure. Where is the harm in letting those that want the procedure to unblock their CCSVI, in getting it? Now it will be "buyer beware" until mainstream medicine "allows" the qualified doctors to perform the procedure. And who knows when this will be... Get screened in the US. Check out http://www.ccsviclinic.ca/ for more information. Call (404)461-9560 to schedule your pre- and post procedure screening today in Fargo, ND. You can also email them at apply@ccsviclinic.ca.
The smaller wheels make it easier to move the wheelchair in tight spaces, such as an apartment or crowded office.
ReplyDeleteIt should be mentioned that our research is under much scrutiny & attack from elements that are trying to control the industry & the dialogue.We would ask you to have the independence of thought to see through their campaign of deceit. http://www.ccsviclinic.ca/?p=783Regular research updates will be published on the Clinic website. Questions about participation may be directed toward the Clinic administration at 888-419-6855.
ReplyDeleteAn alternate magnificent read is Dr. Ashton Embry's Open Letter to Alberta's Minister of Health, which requires a withdrawal of AHS's August 6 announcement with respect to MS and CCSVI in light of the fact that it was loaded with mistakes and apprehension mongering. Dr. Embry's letter presents research information and truths in regards to CCSVI.
ReplyDelete