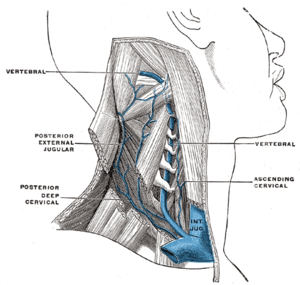
Image via Wikipedia
The subject of CCSVI (the vascular theory of MS) has proven to be incendiary, and has set the MS community ablaze. Initial studies into the hypothesis indicated substantial benefits could be gained by opening up the blocked veins in the neck and thorax of MS patients. These studies were soon backed up by an ever building wave of anecdotal patient reports of sometimes nearly miraculous improvements gained almost immediately after undergoing venoplasty, now known in the CCSVI universe as the Liberation Procedure.
In the wake of these reports, a tremendous amount of controversy has arisen, pitting MS societies and mainstream neurology against patients suddenly energized by hope, clamoring for access to a procedure they believe has a good chance to save them from the unrelenting ravages of the MS beast. Canada, which has one of the highest per capita MS rates in the world, has declined to even allow treatment studies of the liberation procedure to begin. Its single-payer health system refuses to recognize venoplasty as a potential treatment for MS, leaving Canadian MS patients with no options for treatment in their home country. The same situation holds true in most European countries. In the United States, the state of affairs is somewhat better, as an increasing number of physicians are offering the treatment to patients, although many health insurance companies won't cover it, and the cost of treatment is quite high. Additionally, waiting lists can extend for six months or more.
As a predictable result of this pent-up demand for treatment, a flourishing "medical tourism" industry has emerged around CCSVI, with clinics in Poland, Bulgaria, Costa Rica, Mexico, China, and India (and I'm sure I've forgotten a few) offering the procedure for a price, typically between $10,000-$20,000. It's been estimated that somewhere in the neighborhood of 2500 patients have visited these clinics, none of which have tracked the condition of their patients to any acceptable degree once the patients have departed for their home countries. Some of these patients have reported in at various sites on the Internet, but these patients probably represent less than 10% of the total patient population treated. Therefore, we have no good data on the effectiveness or safety of the treatments performed abroad.
The Liberation Procedure can take two forms: balloon angioplasty, in which tiny balloons are inserted into the veins and then expanded, thereby forcing open the veins, or stenting, a process involving the insertion of tiny mesh metal tubes into the veins, which when expanded prop the veins open. Often the two methods are used in conjunction, with patients receiving the balloon procedure in some veins, and stents in others. Both procedures carry the risk of clotting, although that risk is much amplified when stents are used. Because of this hazard, those who have undergone the Liberation Procedure are typically required to stay on a regimen of blood thinning anticoagulation medications for several weeks or months afterwards, necessitating the need for careful monitoring by qualified physicians to ensure the proper levels of medication are maintained. This aftercare can sometimes be hard to procure, as many physicians are reticent to treat patients for procedures that have been performed by foreign doctors and that they little understand. This problem has been especially prevalent in Canada, where the single payer health system has thus far refused to provide aftercare to patients that have gone overseas for "liberation".
In recent weeks, several troublesome (and in one case tragic) reports have begun to surface. Some patients returning from treatment in foreign clinics have experienced thrombosis (clotting) in their newly implanted stents, an extremely worrying condition that requires medical supervision (click here for article). In one truly horrifying episode, a young man who traveled to Costa Rica for treatment returned home to Canada, experienced thrombosis, and was turned away by local physicians when he sought their medical expertise. Ultimately, the patient returned to Costa Rica for treatment, and subsequently perished (click here for article). All of the patients in question had stents implanted in their jugular veins, which dramatically increases the chances of thrombosis when compared to balloon angioplasty, although that procedure too opens patients to potential problems with blood clots.
While the above incidents were transpiring, a conference on CCSVI was held at the annual ECTRIMS (European Committee for Treatment and Research in Multiple Sclerosis) in Gothenburg, Sweden. Many CCSVI research studies were presented, which are discussed in detail in the recently released article on Medscape.com (click here for article-you may be required to register at the site for access, a process which only takes a few minutes and is well worth the effort. Medscape is terrific resource for medical information). This article is quite long and offers an in-depth look at some very important research. It should be required reading for all patients interested in CCSVI.
The data presented at ECTRIMS was often in conflict, with some studies contradicting others, but the general consensus seems to be that while there is an identifiable correlation between CCSVI and MS, there is question as to whether CCSVI is the cause of MS. Rather, it may be a condition that is a result of the same disease process that causes the CNS damage seen in Multiple Sclerosis, or very possibly could contribute to the severity of the disease. It's quite possible that all of these scenarios may hold true, as MS differs so much from patient to patient that a variety of factors may result in its causation. In some patients CCSVI may play a major role in their MS, but in others it may play no role at all.
Given the above developments and wealth of new information, I feel compelled to offer the following words of caution. I know this message will not sit well with the most fervent CCSVI advocates, but I feel I would be remiss in not offering them.
While I am still a strong believer that CCSVI will prove to play a major role in unraveling the MS puzzle, I think that it is vital that patients use extreme discretion when choosing whether or not to undergo the Liberation Procedure, particularly if they must fly to far off destinations to procure treatment. According to one of the most experienced physicians performing the liberation procedure, Dr. Gary Siskin in Albany, New York, only about one third of patients treated receive dramatic improvements in their condition. Another third experienced minor benefit, and yet another third received no benefit at all. Furthermore, the rate of restenosis (veins closing back up) after balloon angioplasty is quite high, somewhere in the neighborhood of 50% within 12 months of treatment. These statistics alone should give patients some pause, as 66% of treated patients do not get the level of benefit they hoped for, and of those that do, 50% revert back to their previous condition, necessitating the need for additional procedures. This translates into 17% of patients who get liberated with the balloon method finding the lasting relief they sought.
The use of stents should be seriously questioned. In addition to the news reports above, Internet forums are revealing yet more patients suffering from stent thrombosis, and through this blog I've received numerous e-mails from other patients struggling with this problem. Stent thrombosis is only one of the potential hazards associated with the devices. The long-term failure rates of stents placed in the jugular veins is completely unknown. Most of the stents now being used were originally designed for use in thoracic arteries, where they are not subject to the nearly constant bending, twisting, and torque that they undergo when implanted in the extremely flexible human neck.
Data collected from two other patient populations that commonly receive venous stents (patients suffering from some cancers, and end-stage renal disease patients undergoing dialysis) is not especially encouraging. The failure rate of stents placed in dialysis patients has been found to be close to 50% after one year (click here for study). Although direct comparisons between disparate patient populations cannot be made, this data does provide reason for concern. Thus far, CCSVI patients treated with stents have not reported any instances of stent failure. However, the longest any of these patients have had stents implanted is only about 18 months, and the vast majority of patients fitted with stents have only received them in the last several months. I fervently hope that we do not start seeing a rash of stent failures in the months and years to come. The possibility can't be discounted, though, and only time will tell.
In conclusion, although CCSVI does hold tremendous hope for the future management of multiple sclerosis, we are presently in only the early infancy of investigation into the hypothesis and its relevance to the MS disease process, and of the practice of treating the condition with venoplasy. Beyond a doubt, future Liberation Procedures will bear little resemblance to those being done today, as new devices specifically designed for the task come on market, and the techniques and practices used to implement them are refined.
My heartfelt advice is that all those except the most desperate (and by that I mean patients with extremely aggressive disease who are quickly hurtling towards total disability) simply wait for 6 to 12 months before embarking on a quest for liberation. This will at least give some time for research to begin to catch up to patient expectations, and for physicians to better understand the best methods used to address the venous anomalies being found in MS patients.
I echo the warnings of virtually all of the most prominent physicians in the field, Dr. Zamboni included, that no patient resort to medical tourism in their quest for liberation. The risks of doing so are very real, particularly when the use of stents is involved. Balloon angioplasty is a much safer option, but the high incidence of restenosis means that many patients spending tens of thousands of dollars on treatment in foreign lands will find whatever gains they experienced lost, and will suffer not only from a return of their symptoms, but from broken hearts and broken bank accounts.
I fully understand the almost irresistible pull to get the disease taken care of NOW. I am close to being one of the desperate, if I'm not already there. This is why I chose to undergo a procedure this past March, which revealed a significant venous blockage but was unable to get it opened (mine is a very atypical case; the blockage is caused by a muscle outside of the vein pinching it almost closed). Hope is a powerful intoxicant, one that has been long absent for the vast majority of MSers. But we cannot and must not allow hope to eclipse reason. We all would like to see CCSVI advance as quickly as possible, but unfortunate events such as those recently reported will only provide fodder for those who would see the hypothesis relegated to the dustbin. Stay strong, friends, and act with extreme diligence.

A few things that should be noted...
ReplyDelete1) Canada's health care system is not "nationalized". It is single payer, that payer being the province.
2) If the treatment for restenosis/blood clots is redoing the procedure, doctors in Canada can't do it as it is not an approved procedure. They can monitor the blood thinners, remove the stent in case of an emergency and treat a stroke. That's it.
3) Canada is doing studies on CCSVI - specifically in the diagnostic and imaging issues that come with it. The province of Saskatchewan is doing liberation procedure studies. Saskatchewan will only do the procedure for Saskatchewan residents I have been told.
lori-thanks for the clarifications regarding the Canadian healthcare system. Down here in the US, any system that is not-for-profit is generally called "nationalized". Single-payer is a tremendous bogeymen. I'll make the changes in the post above.
ReplyDeleteI think I make your second point clearly in the post, stating that Canadians traveling abroad for treatment can't get aftercare in Canada.
Also, Saskatchewan has just started the process of selecting out who will conduct the CCSVI treatment trials. It's expected that the trials will start enrolling in April 2011. There are currently no ongoing treatment trials in Canada, though as you say the MS societies of the US and Canada have funded seven trials primarily seeking to prove the correlation between CCSVI and MS…
It's so enjoyable reading your well written posts. I came onto the MS scene when CCSVI was kind of in a crazy place (a whole few months ago) and your site has always been very informative as to "where it is" at the current moment.
ReplyDeleteThe patients lag slightly behind you, and most of the doctors behind the patients.
At this point, I am still the "rational" guy I was then, but now I have caught the urgency bug. I am mad at MS neurologists for not getting on the train. I am frustrated when I realize most doctors don't have the passion required to cure diseases, and in some cases, I have to even be forgiving of that.
Right now it feels like our village has gotten together to build a house but some of the most skilled craftsmen haven't yet committed to the job. I know I have to be nice to them, because I need them, but at the same time, I have a strong urge to go kick them in the butt to get them moving.
I also feel the tension in the air, while I may feel restraint, and I see you trying to keep the peace, I think some of my fellow MSers are about to start a nasty fight, and I can't decide how I feel about that.
It's going to be an interesting year.
I was at the Life with MS conference in Gothenburg held the day before the ECTRIMS began - this was for "care professionals", MSers, MSers' relatives etc. - about 400 participants.
ReplyDeleteWe heard speakers talking about present treatment methods, future treatments and how they are researching for more treatment.
They urged us to be careful regarding CCSVI treatments - they did not dismiss it 100% but argued, that not all aspects regarding that kind of treatment have surfaced. They believe that some theories behind the CCSVI treatment might assist to an even better treatment in the future.
In the lunch break we found out, that discussions between MS'ers in the treatment centers/clinics in Sweden, Norway and Denmark are really intense when it comes to CCSVI - seems like either you are pro or con, not in between (in doubt). Whereas the discussions in Germany and Iceland were more neutral.
I am lucky that TYSABRI works for me making my life with MS somewhat tolerable, but I fully understand why some will look at the CCSVI treatment to "survive" the MS. That makes me one of the neutral MSers believing that this is another attempt in finding a successfull treatment (and someday cure) for MS.
I really like reading your blog on life / thoughts with MS :o)
Thanks so much for your thoughtful insight... My only wish is that you would refer folks to a more useful article.
ReplyDeleteThe Globe and Mail article to which you refer is riddled with errors - in almost every single paragraph! I am very surprised...did you not read it? Here's a more accurate one: http://www.cbc.ca/health/story/2010/11/18/multiple-sclerosis-vein-death-costa-rica-mostic.html
Thanks and keep the faith - and reason!
Sincerely,
A frustrated but liberated Canadian.
Wendy-thanks for spotting that. In the body of my post, I do link to the CBC article you refer to. The "related articles" that follow the post are automatically generated by a blogging tool that I use, and I stupidly didn't check to make sure the suggested articles were appropriate. I'm deleting the offending link now.
ReplyDeleteThanks again for picking up on that…
Hello, Marc,
ReplyDeleteI remember reading about your procedure last march but forgot about this muscle puting
pressure on your vein and reading it this morning reminds me of a FB site who talks about a doctor in Chile who operates people for what he calls Sindrome Operculo Thoraxico (SOT) He removes the escalen muscle and sometimes the first rib in order to make place for a better blood flow in the jugulars. MS patients reports improvements of their condition. I don't know what to think of that. Have you ever heard of this?
The link of the site is :http://www.facebook.com/group.php?gid=189965716774 (SOT y CCSVI Chile)
and the name of the doctor: Dr Raul Poblete a
raulpobletesilva@hotmail.com
Thanks Marc for this well informed article.
ReplyDeleteDr. Zamboni himself doesn't believe in the use of stents. I just have a couple of questions.
Kuwait has approved CCSVI treatment to MS patients and From what I recall there procedure is ballooning (angioplasty) using different size balloons. So, does Kuwait use stents in there CCSVI procedure..?? Last, I've heard Kuwait has a better success rate less that 50% in restensosis. Is this true..???
Thanks,
Bob
Why can not heart surgeons do an angioplasty for CCSVI?
ReplyDeleteSt. Joseph's Hospital along with McMaster University in Hamilton, Ontario are performing a research study funded solely by MS patients. They applied to the MS Society for a grant and were denied. They stated that if correlation between CCSVI and MS is found, they will then move on to a treatment phase.
ReplyDeletehttp://www.stjoes.ca/default.asp?action=article&ID=1647
So one day you learn you have MS, a disease with no cure... but that's ok, cause none of the other diseases has a cure. But with the other diseases there is hope, since what causes them is know and therefore a solution can be found.
ReplyDeleteSince my diagnosis, and given I don't believe in miracles, I've made peace with the fact that my condition is going to deteriorate; I will be lucky if it happens slowly. No known cause = Good luck finding a solution... in a 1,000 years!
And then came a possible cause, with a solution attached to it and over 2,000 anecdotal evidence of it working. I will be an idiot if I don't try it. I believe once an MS patient's mind is set nothing will change it. All what can be done is to give people the tools and the information to do it in the most safe environment, and ensure they get the follow-up needed. (For instance, the government of Ontario should cover the doppler test for patients having done the procedure as it's a way to detect reoccurrence. And maybe vascular specialists in Canada should stop undermining their own knowledge about clots and how to treat them.)
Always a pleasure to read you, Marc!
Patricia
Marc, I agree with everything you said, especially the part about medical tourism. I understand Canadians wanting the procedure need to go outside Canada but I cannot see traveling to say, India or Europe, when the procedure is now being done at a number of places in the US.
ReplyDeleteThe big problem is follow up. Even now, there is no one in my area to do a follow up doppler according to the correct protocol to check for restenosis. I will be traveling back to Tampa to get this done.
My understanding is that flexible stents are being developed specifically for jugular veins and until those are available and well tested, I would not get a stent, even if it was indicated. Rigid stents, as are now being used, do not 'mimic' the vein which is dynamic depending upon your position. For me, the risk-benefit analysis after more than 2 years of research on my own came out pro on the side of venoplasty but con when you get to stents. It's a decision each patient should make after being inform and discussing it with your doctor before the procedure.
This is a difficult post to respond to since I take exception to your warning. When CCSVI was new, you felt the overwhelming need to check it out and have the Liberation Treatment performed on you. Unfortunately, the results were not positive. Now, caution is the recommendation for other desperate MS patients.
ReplyDeleteI feel if you had heard that you should proceed with caution, you would have thumbed your nose at the naysayers. It was only after experiencing the procedure with negative results that the caution is being advised.
If patients feel there is some hope in pursuing this theory, they should go ahead with it. Positive or negative results will rest on their shoulders.
MS patients who are on the way down are desperate to try anything that might make a difference. They should remain cautious, but pursue the possibility of treatment with vigor.
Sorry I'm a downer on this post. It just felt like being advised not to go to Cancun because when you went there it rained. So many of us are willing to take the chance on the weather, because there's a CHANCE Cancun might be sunny and warm. Does that make sense?
Debbie Downer who is looking for an upper
Bob-Kuwait is not using stents, and they are reporting better results as far as restenosis goes. I don't think they've published any research, though, and I'm not sure that they've been doing the procedure long enough to fully assess restenosis. Zamboni was seeing restenosis for up to a year after the procedure was done, sometimes longer.
ReplyDeleteDebbie-of course, I respect your opinion. But the facts of the matter are that I do say if a patient is truly desperate, they should do what they need to do. In my case, my right side is completely paralyzed, and my left side is quickly weakening. I'm looking at being bed ridden in the next 12 months. Even so,when I had my procedure done, I refused the use of stents based on the research I had done. I can assure you, I'd be giving the same advice whether I received benefit from the procedure or not.
Facts are facts, the incidence of stent thrombosis is growing, and restenosis is a fact of life with balloon venoplasty. I'm not saying that patients should forgo treatment forever. The techniques used will be refined and honed over the next 6 to 12 months, as doctors compare notes, and bona fide research results come to light.
Dr. Zamboni himself is cautioning that patients only undergo the procedure as part of a valid clinical trials.
Sorry for being a downer, but I'm giving my honest opinion. I'm not saying folks should wait
five years. Within the next 6 to 12 months the body of knowledge about CCSVI's role in MS, and the best practices to perform the liberation procedure will grow exponentially.
If you can get the procedure done locally, keep away from stents, and have access to legitimate follow-up care, that changes the equation. If you're traveling thousands of miles and paying tens of thousands of dollars to a clinic that is not accountable to you once you fly home, that's quite a different story.
Sorry about the rabid post. I am just so tired of managing my symptoms, pissing my pants, tripping over my feet, and the list continues to build. How long can one "manage symptoms"? AHHHHHHHHHHHHH!!!!!!!!!!!!!! I think I'm becoming desperate.
ReplyDeleteDebbie
I'm among the most fervent CCSVI supporters I know and I have no quarrel with what you have said. quite the contrary, Marc.
ReplyDeletePerhaps I am more liberal in my feeling that qualified specialists should be doing this on a larger scale as long as they join together in tracking results and sharing information to drive the technology as quickly as possible.
I've yet to meet the CCSVI supporter who has not wanted to fully discover all the risks associated with treatment. We want studies we want the truth, we want access.
To have denied follow-up thrombosis management is indefensible, even ardent CCSVI opponents agree with that. Bless them for stepping forward quickly to make that clear, in the face of this tragedy. My heart goes out to his family and loved ones.
Marc,
ReplyDeleteInteresting thoughts as usual. I would add that as the evidence is leaning more and more towards CCSVI not being the cause of MS (see the beiruit study in particular) even those at the fast end of progression need to consider how many of their symptoms "liberation" is likely to improve even IF it is successfully performed.
Thanks for a great article. But given the pace of progress in research into MS - despite the lucrative size of the market estimated at USD 12B
ReplyDelete- do you honestly believe in 6-12 months we will see something new?
I think this is a fantastic article. I am bedridden person I have the paralyzed legs and useless right arm and only about 75% of the left arm. I would give anything in the hope of even a slight improvement. I have been skeptical of this procedure since its announcement. for the past 12 years I have experimental and every MS possibility there was I even used SF 1019 to the tune of $16,000, what a waste. This procedure may have a future by jumping in on it right now you may not. I say give it time and improvement before you jump off the bridge. I will wait as it is I sit waiting for God, not going to go there with a stent in my heart
ReplyDeleteThanks for your great post as usual.
ReplyDeleteJanuary 2010 I recieved my official MS diagnosis. They started trying to diagnose me when I was 25, that was two years ago. As you all know MS is crazy and things get scary pretty fast. So August 31st I went to Mexico from Canada, was tested and had the balloon angioplasty. They found I had two faulty valves one in each jugular vein. I spent a little over $10,000. Since the procedure I have noticed steady improvement every day and have no regrets.
I haven't been an "MSer" for long but one thing that I have gathered is that every descion you make when you have MS is a gamble. For me going to Mexico was the best option. So far it has payed off. Will the faulty valves come back? I doubt it but who knows. I find it unlikely that MS caused faulty valves to reflux blood to my brain, but what do I know? I think it is much more likely that they where just birth defects.
Until some of these neurologists can contain their egos especially in Canada and get to work answering some of these questions MSers will continue to take risks and some will die doing so. Some also die taking gambles on Tysabri and stem cell research though. In the meantime the clock ticks on. My guestimation at the time of my decsion was that in Canada it would take at least 5 years for this procedure to be open to the average Canadian with MS. Is that a time frame you can deal with? I couldn't. Unfortunatley to date nothing has convinced me that this timeline is inaccurate. I'm just saying...it didn't look good, but now it's done I feel great and I have moved on with my life. What a relief!
-R
WHERE did you get your information Kamikaze? My Grandma went to India and got 7 stents. At that time she couldnt walk. Now she is jogging almost 12 miles. She had a great time in India and is taking lots of Cumin and even her Libido has jumped off the charts. You need to review your information.
ReplyDeleteBrent Musberger
mbinon-thanks for that info, I will definitely do some research…
ReplyDeletePatricia-CCSVI does indeed give us hope. But remember, we don't have 2000 anecdotal reports, only a few hundred at most, and not all of those are positive. The vast majority of those who have undergone liberation have not been tracked in any way. It's a real shame, because that information would be of tremendous value…
Ms Andisue -flexible stents designed specifically for use in veins are exactly what is needed. I have to imagine that with the potential money to be made from such a product, designers are hard at work…
Debbie-you have nothing to be sorry about. All views are welcome here, as long as they are presented reasonably politely.
Carol-yes, we all want as much research to be done as quickly as possible. I've no problem if somebody can find a local doctor to perform the procedure, although I do feel that their chances for success would be better if they waited six months or so. We are learning so much more almost by the day…
Anonymous-yes, there is mounting evidence that CCSVI may not be a cause of MS, or might just be among a variety of causes that work in conjunction to create the disease. Either way, I believe it's going to prove to be a large part of the puzzle…
josef vif-thanks for your comments, and although we have seen MS research progress at a snails pace, it shouldn't take too long to reveal whether or not the liberation procedure provides quantifiable benefit to those who undergo it. What we need are several robust treatment studies, and those need not be very long in duration.
Big Bubba-I know from some of your previous comments that MS has you tightly in its grip. Still, you express the heart of the lion. If things are truly desperate, you might want to consider rolling the dice, but only if you can find someone local and not fly thousands of miles to do it.
R-congratulations on your successful procedure. I hope with all my heart that you continue to see improvement, and that your improvements are permanent. Please check in and let us know how you're doing…
Brent-aren't you about 70 years old yourself? You've been announcing football since I was in grade school. That grandmother of yours must be something else, were her stents made of rocket fuel? (To other commenters, "Brent" and I are friends, and as we say here in New York, he's only busting my balls, as good friends do)
in the morning it will be Thanksgiving Day. I am not where I wished to be in this life due to MS. but I intend to greet tomorrow with thanks. I have been wondering in this procedure if they were to use a series of short stents if they would both keep the vessel open in gaps between them allow enough flexibility?
ReplyDeleteWow, I got blasted for daring to suggest CCSVI was yet another decision MS forced me to make, over my 20yrs DX. My questions about it, my doubts, wow did I hear about how unsupportive of the MS community I was and how I like keeping my MS label! YOUR name came up often as someone I should be more like. From your many posts I never thought I was that much different. I wonder what they will think of me now? I won't hold my breath for an apology for being spoken to so harshly. Many of these "desperate" people have not been DX for very long and "JUST MAKE IT GO AWAY!" panic mode seems their call. Well, they seem to look up to you, so I hope your post sinks in.
ReplyDeleteThank you! Through some unfortunate recent incidents, I have had to go without my meds for this month and Ive really had to face the fact that this DAMN disease has affected me more than I care to admit. I have been watching the CCSVI since I learned of it and had just begun seriously searching for places that did it. Thanks to your info, I will be more patient and cautious as I am sure my children would rather have a disabled Momma than a dead one. I doubt that I would find a doctor (a decent one anyways) that would perform the procedure on me as I have already shown issues with my blood clotting too quickly (making the clotting afterwards even more of an issue). Also I have Chiari Malformation. Very well written and informative as usual. Yes it is a hope dashed but I would rather that than get into something and end up in over my head or even dead! Glad to see you up and at it again!!!
ReplyDeleteHave you seen the latest research study that showed that MS is triggered by an environmental pollutant call acrolein, which is found in tobacco smoke and auto exhaust? What I found intriguing is that study showed that the disease is lessened with the drug hydralazine, which is a vasodilator. Maybe the drug can replace the liberation procedure?
ReplyDeleteHere is an article about the study: http://insciences.org /article.php?article_id=9661
Best of luck, Marc: your site helps keep me hopeful.
auto exhaust most interesting. I have smoked some in my life not as much as most, but I worked around vehicles and foolishly suffered carbon monoxide poisoning numerous times. Several times quite severely. I understand ever so completely how people new to MS want to believe the liberation procedure could be the answer. I have been looking for the silver bullet for 12 years, 10 years ago I would've been the first in line. I hope someday there are better procedures and medications for future generation patients. I too had massive hopes for this even though my time is waning I will have to stall my hopes for a bit on this one. The one thing I must try to do is see every day as a blessing and enjoy all I see.
ReplyDeleteMarc,
ReplyDeleteBrilliant as usual. I think the figures on restenosis are improving. Dr. Zamboni said at the American Neurological Association conference that he had reduced it from 47% to 29%, but without further elaboration. The short term figure out of Kuwait is 2%. It is clearly something that a bit more practice should get right.
While I agree with all of your specific caveats, I draw a slightly different conclusion. My wife, an Israeli, was treated in Poland and will be following up with a NYC-based physician you know well in the new year.
The risk-benefit, taking into account as many of the cautions as you list, is not just CCSVI treatment in a clinical trial versus cruising along on treatments that "work" in any real sense.
In fact, we all know that for most patients, the drugs not only don't work, they cause a host of nasty side effects. So the choice is treatment that might work with few adverse effects (your cautions well noted) versus awful meds that we know in fact mostly do not work and cause lots of problems.
Sitting around doing nothing is not really a good option, in my opinion.
I remain skeptical about CCCSVI being a cure or even a treatment and await research to prove there is any long term benefit whatsoever. However, in my research, I've now become disillusioned about the copaxone I'm on, and am relying on exercise to keep me healthy. Seemed to be working for months, having a bit of a relapse now.
ReplyDeleteI can't help but draw parallels between my "exercise has saved me" hubris of my healthy months with the same sounds from CCSVI folks.
I still think the answers lie in healing the myelin and on prevention.
And is it just me, or are a lot of these "we want CCSVI now" people pretty healthy overall? I am worse off than many of them. They make me tired.
I had the ccsvi procedure done last week in Los Cabos, Mexico. I tried to keep my expectations low so I wouldn't be disappointed if I had no improvements. I had two large blockages that were ballooned with 22mm balloons (normal balloons used 16mm). My feet are no longer blue when sitting, I have more energy, and I no longer choke on big bites of food or get "brain freeze" from ice cream or ice cubes. Was it worth the risks to have this procedure? - yes Would I pay the money to do it again? - yes Do I expect to be cured from the illness from this procedure? - no I feel the procedure is a possible treatment just like the 15 different medications/drugs I am / or have been on. I was willing to wait until Canada started doing the procedures, however, I've lost the ability to cough and if I get a cold/pneumonia I'm sure I would not make it. Hopefully this procedure helps restore those muscles! It's like the lottery - some prople will win big, some will win a bit and some won't win anything. We all have the right to make the decision to buy that ticket and take that chance! Some people believe buying that ticket is a waste of money, that's their opinion and their right. If we MS'ers want to buy that ticket that's our choice. One might win big, one might win a little and one might not win at all - but you need to buy that ticket to win.
ReplyDeletehey, i have not read all your stuff, but...what is your diet like? gluten free? dairy free? fresh, organic foods? raw foods? all of these would help you tremendously. If God did not make it, don't eat it. NO high fructose corn syrup, corn sugar, hydrogenated fats...nothing artificial including sweeteners
ReplyDeletehope that helps you some. check out functional medicine, gluten, yeast overgrowth, biofilms, have someone look at your MTHFR, phase I and phase II detoxification...if you live in NY, look up Dr. Mark Hyman...
good luck